Power Standing Wheelchair XO-505 Series
The Standing wheelchair from Karman Healthcare feature state of the art technology that can help change your life. Featuring an easy to access joy-stick controller that allows you to fully control the movement of the chair. It also features a stand up mode, which allows you to drive the chair while in a standing position.
Power Standing wheelchair are typically used for environmental access and pressure relief. You can control the speed of the chair through the easy to access joy-stick controller, which is positioned perfectly within reach of any type of user. You can easily adjust the length of the arms in order to better suit your needs.
You can also adjust the backrest and even fold it down in order to easily store it in any type of [large] vehicle. You can also control the angle at which the chair will lock into with the joy-stick controller, you can adjust it from sitting mode like any regular wheelchair, all the way to standing mode and anywhere in between. These chairs also feature our top of the line Memory Foam Seat Cushions, which comes standard with every stand up wheelchair.
Stand-up wheelchair series are designed for comfort and durability; they are also very economical alternatives to other stand-up wheelchairs on the market that can cost upwards of tens of thousands of dollars. Our standing wheelchairs offer many health benefits, including improvement of blood circulation, kidney and bladder functioning, as well as improvement of muscle tone. Standing wheelchairs are powered by two (12v) batteries that can run for a long period of time, and last for a range of 25 miles.
- Standing wheelchair is CE Approved / USA Patent: 7,097,189 B2
- Standing chairs are made from 6061 T-6 Aircraft-grade Aluminum Frame
- Standing wheelchairs come stock with flip-back armrests w/ clear plexiglass side panels
- Most affordable stand-up wheelchair in the market
- Increased Pressure Relief Improved functional reach to enable participation in ADL
- Improved Circulation, Enhance independence and productivity
- Improved Respiration, Maintain vital organ capacity, Reduce occurrence of UTI
- Improved Flexibility, Maintain bone mineral density, Improve passive range motion
- Improved Ease of Transfer, Reduce abnormal muscle tone and spasticity, pressure sores
- Reduce the pressure sores, skeletal deformities, and psychological well being
- Raises Independence
- Raises Self Esteem
- Heightens Social Status
- Allows For Easier Communication
- Extends Access Level
- Improved Quality of Life
- Optional Headrest
- Optional Attendant Controller
- Optional Tray Model / Dual Model
- Optional Junior Model 14″ seat width
- New motor launch by Lloyd Actuator / Motor, Dec 2010 discontinued Denmark Linak Motor
- Improved Quality, and new Models coming soon in this category including recline and tilt!
SCI Model Systems
Presently, there are 14 systems and 5 Form II centers sponsored by the National Institute on Disability and Rehabilitation Research, Office of Special Education and Rehabilitative Services, U.S. Department of Education.
The Spinal Cord Injury Model Systems Slide Show
The Spinal Cord Injury Model Systems Slides (PDF version)
MSKTC SCIMS Flyer
Model System Knowledge Translation Center Website
| UAB Model Spinal Cord Injury Care System University of Alabama at Birmingham, Birmingham, AL 205-934-3283 sciweb@uab.edu |
Visit Website | |
| Southern California Spinal Cord Injury Model System Rancho Los Amigos National Rehabilitation Center, Downey, CA 562-401-8111 SCIMS@larei.org |
Visit Website | |
| The Rocky Mountain Regional Spinal Injury System Craig Hospital, Englewood, CO 303-789-8306 Susie@craighospital.org |
Visit Website | |
| South Florida Spinal Cord Injury Model System University of Miami, Miami, FL 305-243-9516 dcardenas@med.miami.edu |
Visit Website | |
| Georgia Regional Spinal Cord Injury Care System Shepherd Center, Inc., Atlanta, GA 404-350-7591 lesley_hudson@shepherd.org |
Visit Website | |
| Midwest Regional Spinal Cord Injury Care System (MRSCIS) Rehabilitation Institute of Chicago, Chicago, IL 312-238-6207 mkaplan@ric.org |
Visit Website | |
| Kentucky Regional Model Spinal Cord Injury System Frazier Rehabilitation, Louisville, KY 502-582-7443 degrav01@louisville.edu |
Visit Website | |
| New England Regional Spinal Cord Injury Center Network Boston University Medical Center, Boston, MA Gaylord Hospital, Wallingford, CT Hospital for Special Care, New Britain, CT 617-638-7380 bethlyn.houlihan@bmc.org |
Visit Website | Visit Website |
| Spaulding-Harvard Spinal Cord Injury System Spaulding Rehabilitation, Boston, MA 617-573-2862 SpauldingHarvardSCIMS@partners.org or hls15@partners.org |
Visit Website | |
| University of Michigan Model Spinal Cord Injury Care System Ann Arbor, MI 734-763-0971 model_sci@umich.edu |
Visit Website | |
| Northern New Jersey Spinal Cord Injury System Kessler Foundation Research Center, West Orange, NJ 973-243-6973 abotticello@kesslerfoundation.org |
Visit Website | |
| Regional Spinal Cord Injury Center of the Delaware Valley Thomas Jefferson University, Philadelphia, PA 215-955-6579 marilyn.owens@jefferson.edu |
Visit Website | |
| University of Pittsburgh Model Center on Spinal Cord Injury Pittsburgh, PA 412-232-7949 greekk@upmc.edu |
Visit Website | |
| Northwest Regional Spinal Cord Injury System University of Washington, Seattle WA 800-366-5643 nwrscis@u.washington.edu |
Visit Website | |
Form II CentersThese centers were previously funded Model Systems and continue to collect Form II follow-up data. New participants are not enrolled. |
||
| Santa Clara Valley Medical Center San Jose, CA (408) 885-2383 Kimberly.Bellon@hhs.sccgov.org |
Visit Website | |
| Mount Sinai School of Medicine New York, NY 212-659-9369 james.cesario@mssm.edu |
Visit Website | |
| The Institute for Rehabilitation and Research (TIRR) Memorial Hermann Houston, TX 713-797-5972 Michelle.Feltz@memorialhermann.org |
Visit Website |
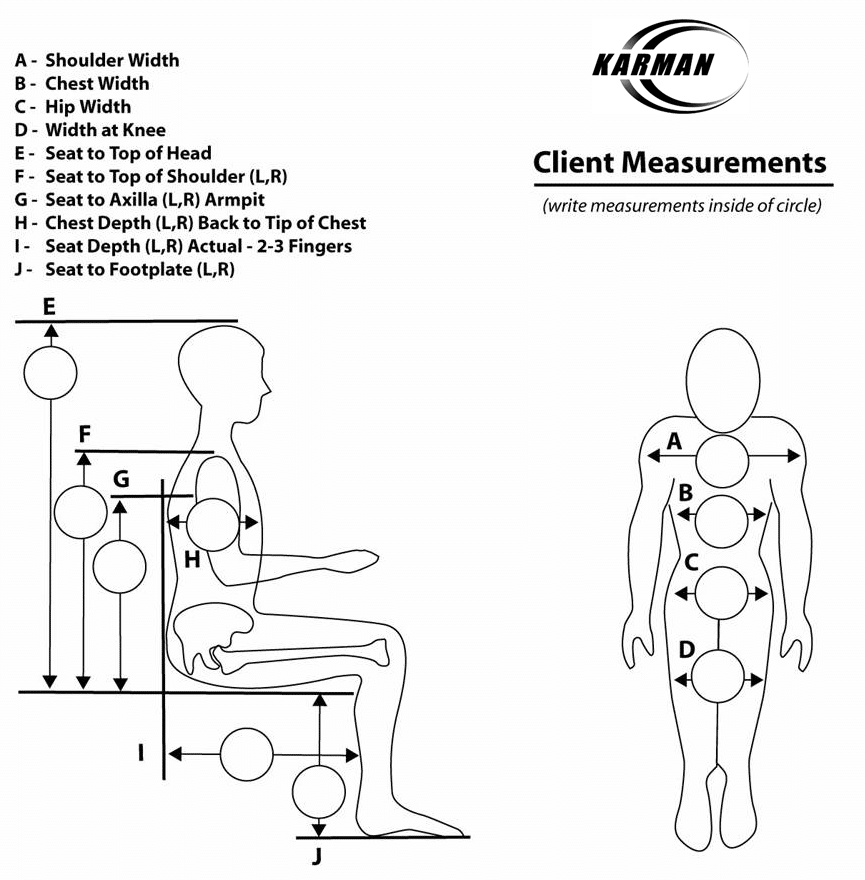
Finding the Perfect Wheelchair to FIT YOU is very important. That is why we have launched the new ERGO FIT™ Campaign based on proper Wheelchair Ergonomics, comparing and contrasting both your body’s needs, your Wheelchair Dimensions, and also balancing the environment in which you will be enjoying your wheelchair.
Whether it is outdoors expeditions and ensuring that going up a ramp with the least amount of resistance, or being as comfortable as possible due to prolonged usage, our ERGO FIT™ methodology provides a countless amount of options and accessories, or models with specific variations designed to maximize your mobility and comfort.
RESOURCES – Each Product Landing Page has all the information pertinent to the product (e.g. HCPCS Codes, Dimensions, Literature, UPC, etc). If you would like to see every product listed by specs and details, please visit our Resources Landing page by clicking HERE. Check out our Landing Page Directory.
What is a Spinal Cord Injury ?
A spinal cord injury (SCI) is generally described as damage or trauma to the spinal cord that has resulted in lost and/or impaired function resulting in reduced mobility and/or feeling.
Common causes of damage to the spinal cord are trauma (car/motorcycle accident, gunshot, falls, sports injuries, etc.), or disease (Transverse Myelitis, Polio, Spina Bifida, Friedreich’s Ataxia, spinal cord tumor, spinal stenosis, etc.). This damage to the spinal cord is known as a lesion, and the paralysis is known as quadriplegia if the injury is in the cervical (neck) region, or as paraplegia if the injury is in the thoracic, lumbar or sacral region.
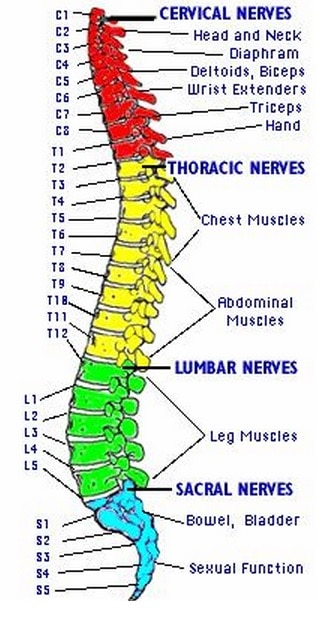
The spinal cord injury level is usually referred to alpha numerically, relating to the affected segment in the spinal cord, ie, C7, T10, L3 etc.
Below the conus medullaris (L1-L2), the spinal canal contains a mass of nerves referred to as the cauda equina or “horse-tail”. These spinal nerves divide off the lower end of the spinal cord and contain the nerve roots from L1-5 and S1-5. Injury to these nerve roots are referred to as cauda equina syndrome.
It is possible for someone to suffer a broken neck,or a broken back without becoming paralysed. This occurs when there is a fracture or dislocation of the vertebrae, but the spinal cord has not been damaged.
Complete and Incomplete Spinal Cord Injuries
There are typically two types of lesions associated with a spinal cord injury, these are known as a complete spinal cord injury and an incomplete spinal cord injury. A complete type of injury means the person is completely paralysed below their injury. An incomplete injury, means only part of the spinal cord is damaged. A person with an incomplete injury may have sensation below their lesion but no movement, or visa versa. There are many types in incomplete spinal cord injuries, and no two are the same.
Such injuries are known as Brown Sequard Syndrome, Central Cord Syndrome,Anterior Cord Syndrome and Posterior Cord Syndrome.
Spinal Cord Injury Rehabilitation
Rehabilitation for individuals with a spinal cord injury combines physical therapies with skill-building activities. These activities will usually take place at a specialist center such as a spinal cord injury rehabilitation center or spinal injury center. A rehabilitation team will usually oversee activities and include a doctor specialising in spinal injuries, social workers, physical and occupational therapists, sports educators, rehabilitation nurses, rehabilitation psychologists, vocational counselors and nutritionists.
Generally, a paraplegic will be in hospital for around 5 months, where as a quadriplegic can be in hospital for around 6 – 8 months. Both paraplegics and quadriplegics should have some kind of rehabilitation and physiotherapy before they are discharged from hospital, to help maximise their potential, or help them get used to life in a wheelchair, and to help teach techniques which make everyday life easier.
Disabled sports, and wheelchair based sports can be an excellent way to build stamina, and help in rehabilitation by giving confidence and better social skills. The ultimate reward for many disabled sportsmen and women, is to win at the paralympic games, which will be coming to London in 2012.
Spinal Cord Injury Cure and Treatment
A cure for long term paralysis is still some years in the future, but clinical trials are taking place with olfactory ensheathing glial (OEG) cells and embryonic stem cell based therapy.
Quadraplegic, Tetraplegic, Paraplegic and it’s Definition
Quadraplegic is derived from two separate words from two different languages, Latin and Greek. The word “Quadra”, meaning “four” which is derived from Latin, relates to the number of limbs. “Plegic”, is derived from the Greek word “Plegia”, meaning paralysis.
Put the two together, and you have “Quadraplegia”.
“Tetra” is derived from the Greek word for “Four”. “Para” is derived from the Greek word for “two” Hence: Tetraplegic and Paraplegic.
In Europe, the term for 4 limb paralysis has always been tetraplegia. The Europeans would never dream of combining a Latin and Greek root in one word.
In 1991, when the American Spinal Cord Injury Classification system was being revised, the definition of names was discussed. The British are more aware of Greek versus Latin names. Since Plegia is a Greek word and quadri is Latin, the term quadriplegia mixes language sources. Upon review of the literature, it was recommended that the term tetraplegia be used by the American Spinal Cord Association so that there are not two different words in English referring to the same thing.
Check our bestsellers!
Motorized Wheelchairs
Active Wheelchairs
Motorized Wheelchairs
Motorized Wheelchairs
Motorized Wheelchairs

















































